Nursing Tips for Treating Patients with Substance Use Disorders

Nobody is immune to developing Substance Use Disorder (SUD). It can affect anyone of whatever culture, age, gender, financial condition, or line of work. Patients who abuse potentially addictive substances pose a widespread and growing challenge to the nursing profession. The behavior that results from this disease has far-reaching and negative effects on the patients themselves, their families, and society. The nurse’s recognition, understanding, and non-judgmental compassion toward patients with substance use disorder are crucial for establishing trust, a therapeutic bond, promoting effective treatment, and facilitating the road to recovery.
What is Substance Use Disorder?
SUDs are brain disorders resulting from long-term exposure to potentially addictive substances such as illegal drugs, excessive alcohol, or even misused prescription or over-the-counter medications and from subsequent mental and physiological dependence.
The consequences can be seriously damaging to social and family life, academic and work performance, as well as general health. It can also be life-threatening.
The terms substance abuse, addiction, and drug dependence all tend to convey and confirm stigma and rejection. To address this issue and promote more understanding and compassion regarding excessive substance use, the 2013 publication of the 5th edition of the Diagnostic and Statistical Manual of Mental Disorders (DSM), the official guide for diagnosing behavioral disorders, introduced the term substance use disorder (SUD), which has levels ranging from mild to severe. Addiction is the most severe form of SUD, involving continued substance use in spite of negative consequences.
Using the phrase “Substance Use Disorder” is more appropriate because it acknowledges the underlying complexities and challenges individuals face, whereas the word “abuse” implies that the person can control and change this behavior on their own without help.
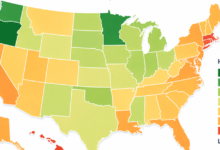
How Many Americans Have a Substance Use Disorder?
The National Survey of Drug Use and Health revealed that in 2021 over 46 million Americans over age twelve had a SUD, that is 16.5% of the population. 29.5 million had alcohol use disorder, 24.0 million had drug use disorder, and 7.3 million experienced both.
Sadly, 94% of those with substance use disorders did not receive any treatment. Historically, services for preventing and treating SUD were separate from general healthcare and mental health services. These issues were often seen as social or criminal problems, and treatment options were limited and rarely covered by insurance.
To address SUD effectively, it is vital to integrate prevention, treatment, and recovery services into healthcare systems. This integration aims to improve access to quality treatment, reduce health disparities, and lower costs to society. Recent healthcare reform laws and evolving trends in the medical landscape are facilitating this integration and striving to better serve individual and public health.
How many patients admitted to the hospital have substance use disorder?
Between 2014 and 2018, an average of 9.4% of the patients visiting emergency departments (9.3 million visits) and 11.9% of the hospitalizations (1.4 million) were suffering from alcohol or substance use disorders (AUD or SUD).
According to this study, the substance abuse rate in adult patients is 1 in 11 emergency department visits and 1 in 9 hospitalizations.
A Sad story
The Journal of Addiction Medicine published the story of a young woman about to give birth who arrived at the hospital with untreated cocaine and opioid use disorder. She began methadone for her SUD and had arranged to enter residential SUD treatment with her healthy baby after the birth. During transfer to a postpartum room, nurses noticed foil and a lighter among her belongings and called security, as the in-hospital substance use policy suggested. The sheriffs checked for outstanding warrants per their protocol, and seeing that the mother had a parole violation, they arrested her on discharge. Tragically, instead of going ahead with her plan to enter addiction treatment and responsibly parent her child, she left the hospital in handcuffs.
Hospital and nursing policies are evolving, and Nursa supports the nurses’ dedicated efforts to accompany and aid SUD patients in their pursuit of recovery and to avoid further harm to all patients, even in the most trying cases.
How to Help Patients with SUD
Many nurses ask themselves how to care for patients with substance abuse problems. The DSM says to start by acknowledging it as a substance use disorder that urgently calls for compassionate and understanding attention. Recognizing the signs can guide you onto the right track.
Signs of SUD
Other than screening that the hospital may or may not perform on patients, a nurse may observe some of the following signs or symptoms to detect this condition:
- Confusion
- Neglecting to eat
- Mood swings, irritability, or sudden changes in behavior
- Antagonism or denial when confronted about SUD
- Withdrawal symptoms when the person decreases or stops using the drug, such as tremors, sweating, or restlessness.
- Reports or comments from family members, friends, or other caregivers regarding the patient’s substance use or related behaviors.
- Fearful or secretive behavior, with no reason except to hide substance use.
With the complexity and increasing frequency of caring for patients with SUDs, nurses need to be prepared for the various mental states that these patients experience, in general terms, denial, coping, and powerlessness.
How to Be Compassionate as a Nurse
Tips for Nurses Caring for Patients with SUDs
Once you recognize two or more signs of SUD, you will realize that this patient needs special attention. A few simple, but not always easy, tips maybe offer some support.
For patients in denial
- A non-judgmental attitude strengthens trust, encourages open communication, and builds a therapeutic nurse-patient relationship.
- Honest and factual answers to the patients’ questions or comments consolidate trust and may empower the patient to face their condition and make well-informed decisions on their treatment and recovery.
- Providing information regarding SUD can be helpful to overcome denial, such as:
- The continuum from occasional, recreational, or health-related use to addiction.
- The nature of SUD as a complex brain disorder rather than a personal failing or weakness, and how substances affect the body, brain, and overall health.
- Psychological and physical dependence on the substance of use, as well as adaptive changes in the brain as it seeks to regain homeostasis.
- Available treatment options, explaining that seeking assistance is a sign of strength.
- Relapse is a common part of the recovery process that can offer an opportunity for patients to gain valuable insights and learn from their experiences.
For Patients with Coping Difficulties
- Encouraging the patient to talk about fears, feelings, and anxiety reinforces empathy and a trusting relationship that will help the patient come to terms with unresolved or even unconscious problems in their lives that contribute to substance abuse.
Read Nurse Challenges In Communication With Patients
- Exploring alternative coping strategies with the patient may provide them with options for managing stress and relationships. Such strategies include stress management techniques, cognitive behavioral therapy, or art therapy as a means of self-expression and emotional release.
- Examining the patient’s history of substance use may allow the patient to recognize situations that triggered substance use, learning to foresee and, if possible, avoid them.
For Patients Feeling Powerlessness
- Supportively prompting patients to identify their areas of control, particularly setting their own boundaries or reducing negative influences in their recovery, can encourage them, despite past relapses.
- Focusing on the patient’s strengths and resilience begins to restore a sense of empowerment, with patients recognizing their positive qualities and internal resources.
- Celebrating milestones and any successes along the recovery journey fosters a positive mindset, even if the only accomplishment is overcoming denial.
A complex mental health and brain condition, substance use disorder impacts the decision-making ability and definitely makes it hard to stop taking the substance, even if the individual wants to. A trained nurse can help guide the patient to the treatment they need, empower them on their journey, and change the story of their lives.