Ready for the Seasonal Uptick in COVID-19 Cases?

Hospital intake is rising again, and—yet again—an uptick in COVID-19 cases is to blame. Currently, there are two variants of COVID-19 that have people talking: the EG.5 and the BA.2.86. Read further for statistical information about hospitalizations, details about the variants, how to stay healthy, and how to prepare.
COVID Statistics in 2023 for Cases and Hospitalizations
We’ve come a long way since the first confirmed COVID-19 case in the US on January 21, 2020. Unfortunately, the mutating nature of COVID continues to create waves that both ebb and flow as does the population’s pandemic fatigue. The Centers for Disease Control and Prevention (CDC) continues to monitor and publish COVID-19 virus data which currently reports an 18.8 percent increase in hospital admissions and, sadly, a 17.6 percent increase in COVID-19 deaths.
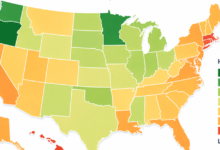
When we look at the data compiled over the past two years, we can thankfully see that even though the virus continues to surge, those surges are less devastating than in prior years. While the rollercoaster of COVID-19 cases doesn’t conform to a strict calendar, there are a couple of generalized patterns. There tends to be an uptick in COVID-19 hospitalizations during the summer months and the end-of-year months into January. We can surely correlate summer swells with increased vacation travels, and the end of the year into January is chock-full of holiday gathering events.
The most crushing billow in COVID-19 hospitalizations occurred in January of 2022, with weekly hospital admissions peaking at 150,674. Thankfully, the two following surges (June 2022 and January 2023) never rose above 45,000. Available CDC data shows hospitalizations are on the rise again after dropping below 8,000 for the early-mid summer weeks. The first week of August hit 10,454 admissions and continued to rise reaching 15,067 the week of August 19.
Find the Good Nurse Your Facility Needs
About EG.5
EG.5 first appeared in February 2023 and by July it had reached a global prevalence of 17.4 percent. In the US, it rose to become the dominant variant by the first week of August holding 15.4 percent of the share amongst other tracked Omicron variants. EG.5 has amino acid mutations in the spike protein—much like XBB1.5, which was the previous dominant strain. The shared profile is of interest because the spike protein is how the virus enters the cells and may allow the virus to work around a person’s existing immunities.
For now, the global risk level for EG.5 has been qualified by the World Health Organization (WHO) as low. This rating appears to be largely because disease severity has not increased, and symptoms seem to be consistent with those already expected.
About BA.2.86
BA.2.86—also referred to as Pirola—is appearing in the news, but as of August 23, there are only two confirmed cases of this variant in the US. If it’s not contributing to the increased hospitalizations, why are we hearing about it at all? This strain is making the news because it’s considerably different from other variants. It’s believed to be better at avoiding antibodies than EG.5 yet may be less infectious than other variants.
Despite the virus’s notoriety, the CDC doesn’t link this variant to the rise in COVID-19 hospitalizations in the US just yet. As a new variant of significant interest, we can expect more data and follow-up information from the CDC if cases continue to pop up.
Share These 10 Mental Health Resources with Your Nursing Staff
Stay Healthy in the Face of Rising COVID Numbers
How can you keep your staff and yourself healthy right now? We’ve all been experiencing pandemic fatigue for a while now. The first year was grueling, scary, isolating, and frustrating, and our communities’ limits were sorely tested. Now, over three years out from the onset, life is essentially back to how it was before. People happily discarded masks once ordinances were lifted, started traveling, and went back to the office (although many workplaces have retained some work-from-home concessions). That’s not a bad thing; humans, in general, are social creatures, who crave connection and socialization.
In light of the current uptick in COVID-19 cases, consider the following tips to promote the health of your staff as you prepare your facility for increased patient admissions:
- Mental health: Burnout continues to be a struggle for nursing professionals, so share mental health resources with your staff.
- PPE supply: The personal protective equipment (PPE) shortages crippled the morale and safety of both staff and patients in some of the more dire moments of the pandemic. Check that supply is stocked and avenues for further sourcing are available.
- Emphasize the basics: Encourage your friends, family, and staff to be vigilant with basic precautions outside the workplace (i.e., washing hands, hand sanitizer, rapid COVID tests, staying home, and masking when ill).
Prepare Your Facility for Increased Patient Intake
Throughout the roller coaster of the COVID-19 pandemic, staffing has been a particularly frustrating challenge for hospital administrators. Overcoming staffing shortages due to large-scale nurse retirements, nurse burnout, and subsequent vacancies—and sourcing enough nurses to establish safe nurse-to-patient ratios—are challenges in any environment. When those challenges are the backdrop amid a constantly fluctuating patient intake, leveraging technology to source nurses flexibly and economically is a game-changer.
Not only can you use Nursa to find registered nurses (RNs), licensed practical/vocational nurses (LPNs/LVNs), and certified nursing assistants (CNAs) to fill vacancies on a per shift basis, but you can use Nursa to directly increase the number of nurses on the floor alongside an increase in patient intake. Instead of riding out the patient surges with your staff working overtime or on-call, pick up a few extra per diem nurses for those shifts. Per diem nurses and nursing assistants are not long-term hires: They are hired on a shift-to-shift basis. This allows your facility to adjust staffing numbers quickly, reducing the burden on your staff without hiring full-time staff employees only to find yourselves overstaffed and facing serious budget concerns once the surge recedes.
Be responsive, quick, and efficient with staffing by utilizing Nursa. Post shifts for nursing professionals only when you need them. With Nursa, there is no quota for how often you source nurses, nor is there a quota for how many nurses you source. Pay only for the hours worked without worrying about retirement benefits, paid sick leave and vacation time, or lengthy hiring processes. There are RNs, LPNs, and CNAs in and around your communities actively looking to pick up shifts, and Nursa is your connection to them. Register your facility today, and source the nursing professionals your facility needs to be responsive to patient intake.