Report into sickle cell nursing care expected this year

A report calling for improvements in nursing care for patients with the UK’s most prevalent genetic blood condition is due to be published later this year.
The upcoming report, led by the Sickle Cell Society, which represents the interests of people with sickle cell disorder, is expected to demand the NHS commits more specialist nurses to the condition and improve its clinical pathway.
“We know over many decades sickle cell has been underserved and underinvested in”
John James
John James, chief executive of the Sickle Cell Society, told nurses at the Roald Dahl Nurses Conference today that support for people with the condition was still severely lacking two years after the landmark No One’s Listening report was published.
“In 2023, we still have people who don’t know much about sickle cell, and that includes health professionals who think you can catch it,” said Mr James.
“It is a debilitating condition, and it’s not just the crises or episodes of pain that effect people who live with it.
“In London, it is in the top 16 causes of all emergency A&E admissions – and we know it can cause early mortality.”
It was at the event that Mr James announced the report, due to publish in late October or early November.
The report will offer recommendations for the health service on how to improve access to, and the quality of, sickle cell nursing care.
Mr James told Nursing Times that it would put forward a minimum service level for sickle cell nursing, and said that it would reiterate the “underfunded and undervalued” nature of it as a nursing specialism.
“The ratios [of nurses] are still far lower than other [specialisms],” he said.
The report will also provide an overview of the current state of the sickle cell nursing workforce, Mr James said, and what needs to be done to improve the nursing care pathway for sickle cell patients.
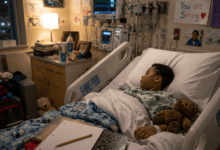
What is sickle cell disorder, also known as sickle cell disease?
Sickle cell disease is a genetic red blood cell condition. It affects haemoglobin and causes red blood cells to form in an abnormal, crescent (or sickle) shape.
This prevents the efficient movement of oxygen around the body and causes build-ups of blood cells. In turn, this can cause respiratory difficulties, severe pain and fatigue.
Sickle cell crisis is when a patient with sickle cell disease experiences acute symptoms or complications relating to the disease. It is a medical emergency, and can cause extreme pain and more severe versions of their chronic symptoms.
Patients experiencing sickle cell crisis, according to National Institute for Health and Care Excellence (NICE) guidance, should be given pain relief, normally in the form of opioids such as morphine, within 30 minutes of A&E admittance.
Best practice then states they should be treated with a patient-controlled analgesia (PCA) pump, which gives them constant background doses of morphine and allows the patient to administer bolus doses for when the pain becomes unbearable.
The use, set up and monitoring of these pumps requires specific training for nurses.
The disease affects around 15-17,500 people in the UK. The vast majority are of Black African or Caribbean ethnicity.
Clinical guidance from the National Institute of Health and Care Excellence (NICE) states that, when a patient presents at A&E experiencing sickle cell crisis, they should receive strong painkillers, often morphine, within 30 minutes of admission.
However, structural racial discrimination towards people with the condition has, historically, led to underinvestment and lack of awareness – including among healthcare professionals – about sickle cell, Mr James explained.
This has led to delays in treatment and, in some cases, deaths.
He said: “We know over many decades sickle cell has been underserved and underinvested in.
“We produced the No One’s Listening report because we were aware of a number of avoidable deaths in NHS hospitals and despite many deaths over the years and coroners being involved, it seemed to be just getting worse.
“[The report] highlighted sub-standard care on general wards and in A&E; whether you lived in London, Manchester, or anywhere else, there were huge variations in the quality of care people received.”
No One’s Listening was published in November 2021 by the Sickle Cell Society and the All-Party Parliamentary Group on Sickle Cell and Thalassaemia.
It came in response to the death of 21-year-old Evan Nathan Smith, whose inquest found evidence that clinicians – including nurses – did not recognise his symptoms were related to sickle cell.
Mr Smith reportedly dialled 999 from his hospital bed to request oxygen after a nurse denied it to him.
The report highlighted the prevalence of deaths, near misses and the difficulties patients experienced in getting the care they needed when presenting in sickle cell crisis.
Mr James said there remained a lack of compliance with national care standards, and that 80% of NHS trusts at the time were missing the 30-minute pain relief requirement set out by NICE.
“People might blame Covid, but [trusts] haven’t been meeting [the guidelines] for decades,” he continued.
“It’s not the pressure A&E departments are facing, it’s something they haven’t met for many, many, many years.
“The consequence is that there is a fear and avoidance of hospitals by people living with the condition. The experience of going to hospital was poor, and that’s putting it mildly.”
“Race was a factor,” he continued.
“Wherever you lived, patients said if they had regular crisis and were in pain went into A&E often, they were somehow drug-seeking, seeking another hit.
“This condition predominantly affects people of colour, and in our view, there has been a lack of investment, a lack of support, and a factor in that lack of support is because this is a group of people who experience racism.”
Mr James said it was important to “not shy away” from this.
Failures to provide joined-up care and huge gaps in community follow-up care after discharge were also found.
Two years since the report, Mr James said the “inadequate” levels of sickle cell training among health professionals remained, but pointed to a promise from the Nursing and Midwifery Council (NMC) to make improvements.
Mr James finished that there were more treatments being developed for sickle cell, but that groups such as his, and the parliamentary group formed to investigate care for the condition, would continue to “raise questions” to keep the issue alive.