Warning lack of line flushing leading to ‘under delivery’ of IV antibiotics
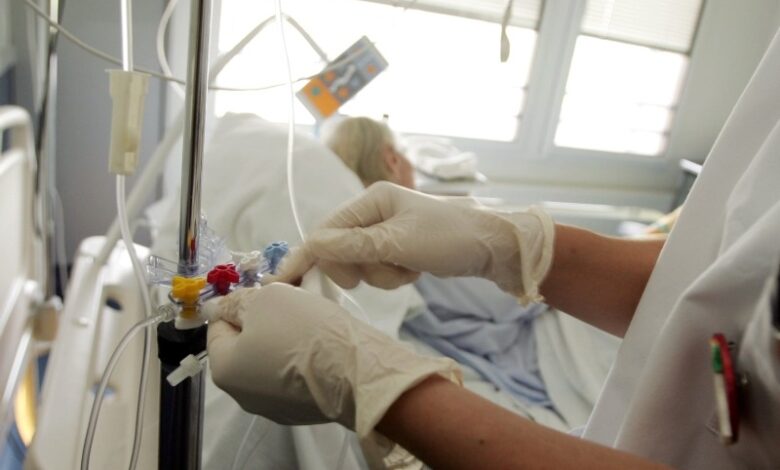
The under delivery of intravenous antibiotics in some NHS hospitals due to lack of polices and compliance may be contributing to antimicrobial resistance (AMR), according to a parliamentary report.
Findings in the report indicated that many health service organisations do not have policies in place to reduce the risk of under delivery and those that do can struggle to comply fully with them.
“Being a nurse puts me in a unique position to be able to understand the impact that under-dosing can have”
Ashleigh Hughes
The report’s authors warned that the residual volume of antibiotic remaining in the line of the IV administration set can result in under delivery of up to 30% of the prescribed dose.
They said that, as a result, this could be leading to possible resistance within patients, owing to the accumulative effect. Nurses involved with compiling the document have called for action.
The report was compiled by the office of Baroness Bennett of Manor Castle and summarises findings from a study of antibiotic ‘line flushing’ and disposal practices in NHS organisations across the UK.
This study, by Dr Paul-Enguerrand Fady, senior parliamentary researcher in Green Party peer Baroness Bennett’s office, was based on Freedom of Information responses from 117 NHS organisations.
Dr Fady investigated the phenomenon of residual volume of antibiotics that remain in the IV administration set (pump or gravity) if a post-medication flush is not administered.
His research investigated how many NHS acute organisations in the UK have specific policies in place surrounding flushing patients’ lines when they give adults antibiotics.
Lack of it can cause the patient to be under dosed by up to 30% of the prescription, noted Dr Fady in his report, resulting in not only considerable wastage to the NHS, but also a hidden cause of AMR.
In addition, he noted that it can also negatively impact the time frame with which a patient could be moved to oral antibiotics, further exacerbating the issue of unnecessary wastage of IV antibiotics.
Dr Fady’s research indicated that around 70% of NHS organisations do not have any administration set flushing policy in place to ensure patients receive the complete dose of antibiotics as prescribed.
It also found that only around 5% of the NHS organisations that responded to the FOI reported that they do flush the IV set routinely, in all clinical areas, administering the total prescribed dose.
Of the 30% of NHS organisations that responded that do have a policy in place, fewer than half said they were fully compliant with their own policy.
Based on the findings, the report recommended that all NHS organisations implement line flushing policies by late 2024, with support from the Department for Health and Social Care.
The report also recommended that national regulators, such as the Care Quality Commission, integrate adherence to line flushing policies into their assessment of hospitals trusts.
In addition, it called for proper training be provided on how to dispose of antibiotics appropriately and that hospitals monitor environmental antibiotics contamination, both in effluent and on wards.
Further recommendations include making funding available to enable research into underdosing’s impact on drug-resistant infections and environmental AMR.
The report – titled Antibiotic under-dosing and disposal in NHS – was launched last week in the House of Lords during an event attended by representatives from the sector, industry, NHS and parliament.
Commenting on his findings, Dr Fady said: “The issue of underdosing is relatively unknown, and is a simple and easy fix to help us tackle the growing pandemic against AMR.”
Ruth Dando, head of nursing for theatres, critical care and anaesthetics at Barking, Havering and Redbridge University Hospitals NHS Trust, was among the nurses that spoke at the report’s launch.
She said: “As a nurse, it is in my inherent desire to do the right thing when delivering clinical treatments and care to patients.
“With the launch of this report we – as an industry – have an opportunity to not only keep our patients safe and well, but to contribute to the ongoing fight against AMR that we are facing.
“The practice is being implemented throughout my hospital trust and I would encourage anyone working in a hospital setting to do the same moving forward,” she said.
Ashleigh Hughes, senior sister at The Newcastle upon Tyne Hospitals NHS Foundation Trust said: “It was a pleasure to speak at the launch of this report in the House of Lords.
She added: “Losing a parent to an incurable disease is heartbreaking, but to know that underdosing of antibiotics shortened the time she had left and it could have been prevented is devastating.
“Being a nurse puts me in a unique position to be able to understand the impact that underdosing can have – and having it highlighted in this way shows all the more why this should be a focus for Hospital policy teams as we move forward.”



